by Dr. Jacqueline Ansel, DVM, MVetSci
Dental health in cats is one of the most common and most overlooked medical and hygienic places on a cat. Dental disease is a medical condition which can develop in cats if their dental health is not maintained. In fact, did you know that the majority of cats over the age of three show signs of periodontal disease.
Cats are masters at hiding pain. That means dental disease often progresses silently, affecting comfort, appetite, and overall health long before obvious symptoms appear.
As a veterinarian, I frequently see cats whose dental discomfort has been mistaken for “picky eating” or “just getting older.” The truth is, feline dental disease can significantly impact quality of life and it’s far more manageable when caught early.
How Dental Disease Affects Cats
Dental disease in cats begins with plaque buildup along the gumline. Without intervention, plaque hardens into tartar, leading to gingivitis (gum inflammation), periodontal disease, and eventually infection or tooth loss.
Because cats are naturally stoic, the signs are often subtle.
Common symptoms of dental disease in cats include:
- Reduced appetite or food refusal
- Dropping food or chewing on one side
- Weight loss
- Bad breath (often more noticeable than owners realize)
- Pawing at the mouth
- Hiding, irritability, or decreased interaction
- Preference for soft food over dry food
It’s important to understand that dental disease is not just about the mouth. Oral bacteria can enter the bloodstream and contribute to inflammation affecting the heart, kidneys, and liver. Chronic dental inflammation may also worsen existing kidney disease, a common concern in aging cats.
Left untreated, dental disease in cats becomes painful and progressive.
Unique Dental Conditions in Cats
Cats are particularly prone to a painful condition called tooth resorption. This occurs when the body begins breaking down the tooth structure itself, often below the gumline.
Tooth resorption:
- Is extremely common in adult cats
- Cannot be diagnosed without dental radiographs
- Often appears normal on the surface
- Requires extraction for relief
Many cats suffering from resorptive lesions appear outwardly normal until advanced disease is discovered on X-rays.
This is one reason routine dental exams and professional dental care are so important in feline patients.
At-Home Dental Care for Cats
Daily dental health for cats can be challenging, but even small, consistent efforts make a meaningful difference.
Helpful at-home dental options include:
- VOHC-approved dental wipes
- Feline-specific toothbrush and enzymatic toothpaste
- Dental diets designed to reduce plaque
- Water additives (when tolerated)
When choosing dental products, look for the Veterinary Oral Health Council (VOHC) seal. This ensures the product has been tested and shown to reduce plaque or tartar.
Pair dental care with a positive reward, gentle praise, petting, or a favorite activity to help reduce stress. Consistency matters more than perfection.
If brushing isn’t possible, don’t give up. Partial plaque control is still better than none.
Professional Dental Care for Cats (COHAT)
Most cats will require professional dental cleanings during their lifetime. These procedures are called Comprehensive Oral Health Assessment and Treatment (COHAT).
Because up to two-thirds of each tooth lies beneath the gumline, dental radiographs are essential for identifying disease that cannot be seen during a visual exam.
Prior to anesthesia, pre-operative bloodwork is performed to evaluate organ function and ensure safety. During the procedure, cats are placed under general anesthesia so a complete, pain-free examination and cleaning can be performed while vital signs are closely monitored.
A feline COHAT includes:
- Full-mouth dental radiographs
- Probing and charting of every tooth
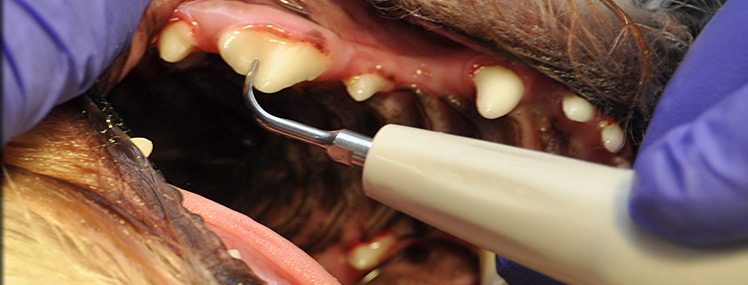
- Ultrasonic scaling to remove plaque and tartar
- Polishing to smooth enamel and reduce future buildup
- Extractions when necessary
Anesthesia is often a concern for cat owners. Modern veterinary anesthesia is highly monitored and tailored to each patient’s health status. The risks of untreated dental disease often outweigh the risks of a properly managed anesthetic procedure.
Extractions: Why Removal Can Be the Kindest Option
Cats frequently require extractions, especially with advanced periodontal disease or tooth resorption.
While the idea of tooth removal can feel alarming, cats typically experience significant relief afterward. Once painful teeth are removed and inflammation resolves, many owners report:
- Improved appetite
- Increased energy
- More social behavior
- Better grooming habits
Cats adapt remarkably well — even after multiple extractions.
How Often Should Cats Have Dental Exams?
All cats should receive an oral exam during their annual veterinary visit. Senior cats or those with known dental disease may require evaluations every 6 months.
If you notice any change in eating habits, behavior, or weight, a dental exam should be part of the diagnostic plan.
Early intervention is always easier and less costly than treating advanced disease.
The Takeaway: Protecting Your Cat’s Oral Health
Dental disease in cats is common, painful, and often hidden but it is highly manageable with the right approach.
A combination of:
- Routine veterinary dental exams
- Professional cleanings when indicated
- Consistent at-home dental support
…can protect your cat’s comfort, behavior, and long-term health.
Healthy teeth are not cosmetic. They are foundational to your cat’s overall well-being.